Simulating the best care
LAU Simulation Center gives health sciences students and visiting professionals an edge over their peers.
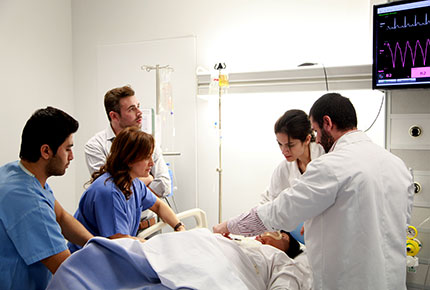
A heavily pregnant woman called Mountaha Droubi has been admitted to hospital complaining of a bad headache. As two doctors take in the details of her ailments, she is crippled by stomach pain and becomes disoriented. When the expectant mother begins to convulse, the doctors know they must react quickly to save her life and that of her baby.
Droubi is displaying the typical symptoms of preeclampsia, a condition where pregnant women develop high blood pressure and protein in the urine. Although preeclampsia is a serious condition, Droubi’s case is not. That’s because she isn’t actually a real person but a high-fidelity human mannequin called Noelle. She is just one of several sophisticated mannequins at LAU’s state-of-the-art Simulation Center, which opened earlier this year.
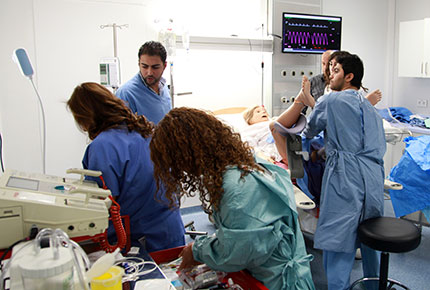
The center’s full-body mannequin simulators are a key learning tool in the Schools of Medicine, Nursing and Pharmacy. Capable of simulating physiological changes such as a loss of pulse, a sudden drop in blood pressure or pupil dilation, the mannequins can be used to simulate a range of scenarios from injections, infant delivery, heart attacks or stab wounds. “LAU is one of the regional pioneers to use simulation in teaching, which is now a requirement for most medical schools in the U.S.,” said Dr. Vanda Abi Raad, associate professor of Anesthesiology at the School of Medicine and co-director of the LAU-Clinical Simulation Center, along with Dr. Nadia Asmar, assistant professor of Medicine.
While Noelle might not really be alive, students and medical professionals are urged to treat her as a real patient. “On reflection I realize we didn’t communicate proper explanations to Mrs. Droubi,” said Christian Etel, one of dozens of practicing doctors from across Lebanon and the region who was at LAU on December 6 to participate in a professional simulation training workshop, “Emergency Situations in Obstetrical Anesthesia”, organized jointly by the Lebanese Society of Anesthesiologists and the LAU-Clinical Simulation Center. He and his colleague Mariette Karam did not have the benefit of using high fidelity simulators while studying. “Some scenarios are better not to practice on a real patient because you could make a major error with a lasting impact,” said Karam. “What’s great about the mannequins here is they really do simulate the symptoms of an actual person whilst protecting real patients from risk.”
LAU’s “very impressive” Simulation Center reflects a commitment to promoting interprofessional teamwork and decreasing human medical errors, said the workshop’s leader Dr. Alexandre Mignon, director of iLUMENS (Laboratoire Universitaire Médical d’Enseignement Numérique et Simulation) and a professor of Anesthesiology and Critical Care Medicine at Université Paris Descartes. “In medicine we work in teams, which means we have to communicate well and anticipate the situation. Simulation allows us to work on our technical skills and our communication in a safe and immersive way.” Mignon led the workshop along with Paris-based anesthesiologist, Dr. Thibaut Rackelboom.
Proper communication can be the difference between life and death in the healthcare profession. According to U.S. healthcare accreditation organization The Joint Commission, inadequate communication between healthcare workers or between workers and patients is the primary cause of over 50% of serious errors in hospitals. Between 44,000 to 98,000 deaths a year in the U.S. are caused primarily by medical mistakes during treatment, according to the Institute of Medicine. “Bad medical practice costs a lot, so simulation is a good way to improve our care. All simulation sessions have a thorough de-briefing session afterwards where the medical professionals can share ideas, discuss errors and think about better ways to practice,” said Mignon.
As one of the best facilities in the country, LAU’s Simulation Center is set to become a major hub of activity, both for students and experienced professionals. “Our mission is to go beyond the university and to play a national and regional role in healthcare education,” said Abi Raad.
More
Latest Stories
- SOE Launches its Distinguished Scholar Visiting Program with International Guest Dr. Feras Batarseh
- LAU Nursing Camp Opens Eyes, Hearts and Futures
- Meet Dr. Zeina Khouri-Stevens, Executive Vice President for Health Services
- LAU Family Medicine Graduates to Benefit from a Partnership With Nova Scotia
- AKSOB Assistant Professor Shares Her Vision for the Future of Learning
- LAU Simulation Models Celebrate 20 Years of Learning, Leadership and Service
- The School of Engineering Hosts the Lebanese Electromagnetics Day
- LAU Stands Out on the Sustainability Scores